 In ‘Understanding Eating Issues’, I started by stating that: “Eating disorders are rarely just about eating or food. They are serious and complex emotional and physical issues and are often a coping strategy used to deal with deeper, underlying problems or emotional conflicts which may be too painful or difficult to address directly”. However, changing your relationship with food is ESSENTIAL to recovery. You cannot recover without eating. Whether your eating is too rigid, chaotic, or fluctuates between both extremes, developing a healthy relationship with food and restoration of health, weight, and nutrition is imperative.
In ‘Understanding Eating Issues’, I started by stating that: “Eating disorders are rarely just about eating or food. They are serious and complex emotional and physical issues and are often a coping strategy used to deal with deeper, underlying problems or emotional conflicts which may be too painful or difficult to address directly”. However, changing your relationship with food is ESSENTIAL to recovery. You cannot recover without eating. Whether your eating is too rigid, chaotic, or fluctuates between both extremes, developing a healthy relationship with food and restoration of health, weight, and nutrition is imperative.
With a long history of eating disorders, it was difficult for me to even envisage what a healthy relationship with food looked like. What was I aiming for? What was the goal? I like Ellyn Satter’s definition of normal eating:
“Normal eating is going to the table hungry and eating until you are satisfied. It is being able to choose food you like and eat it and truly get enough of it—not just stop eating because you think you should. Normal eating is being able to give some thought to your food selection so you get nutritious food, but not being so wary and restrictive that you miss out on enjoyable food. Normal eating is giving yourself permission to eat sometimes because you are happy, sad or bored, or just because it feels good. Normal eating is mostly three meals a day, or four or five, or it can be choosing to munch along the way. It is leaving some cookies on the plate because you know you can have some again tomorrow, or it is eating more now because they taste so wonderful. Normal eating is overeating at times, feeling stuffed and uncomfortable. And it can be undereating at times and wishing you had more. Normal eating is trusting your body to make up for your mistakes in eating. Normal eating takes up some of your time and attention, but keeps its place as only one important area of your life. In short, normal eating is flexible. It varies in response to your hunger, your schedule, your proximity to food and your feelings.”
I struggled however, to identify when I was hungry and when I had eaten enough. My hunger/satiety cues were really out of whack and I required some extra help to know what to eat, how much to eat, and when to eat. My dietitians have been invaluable in this regard and I recommend that all individuals with an eating disorder see a dietitian who can provide information on nutritional needs and collaborate to devise an appropriate meal plan.
________________________________________________________________
 Please note, that those who have been severely restricting or frequently purging for an extended period of time may be medically compromised or at risk of developing refeeding syndrome when they recommence eating if they are not being monitored closely by their doctor and medical team. Refeeding syndrome can cause severe complications and cardiac arrest so medical observation is important and sometimes a medical admission to hospital may be required.
Please note, that those who have been severely restricting or frequently purging for an extended period of time may be medically compromised or at risk of developing refeeding syndrome when they recommence eating if they are not being monitored closely by their doctor and medical team. Refeeding syndrome can cause severe complications and cardiac arrest so medical observation is important and sometimes a medical admission to hospital may be required.
For more information or referrals, see:
♥ National Eating Disorders Collaboration
♥Eating Disorders Association
♥ Isis
or email the Eating Disorder Outreach Service on [email protected]
________________________________________________________________
My dietitians have worked with me to devise appropriate meal plans throughout the various stages of my recovery. What is a meal plan? Basically, an overview of what I need to eat at each meal in order to meet my nutritional requirements. From that meal plan, we were then able to come up with a menu for the week ahead. 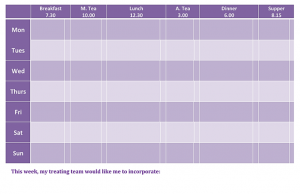 This helped to eliminate decision making at each meal time. Meal times were often emotionally charged times, filled with intense feelings of anxiety and shame. I have found it better to spend 20 minutes planning several days’ meals than 1 hour speculating over one meal. This also allowed me to decide what I would eat away from the anxiety of meal times and ensured I bought the correct quantity of food in advance – so there’s not too little or too much food in the fridge. Initially, my menu was the same day in and day out, and it took quite some time until I was ready to introduce variety into my week. I now enjoy a variety of foods, but on days where things are a little tougher or a little more emotional, I have my basic meal plan which I can fall back on, to ensure my nutritional needs are met. For a blank menu template, click here or on the image above. For each meal time, there is space to write in what you will have, and then a little column/box next to it to tick off once you have completed that meal. I set goals with my treating team of how many ticks a week I will accomplish and then set rewards for metting these targets. I love playing board games, so my current reward is a new game when I sustain one month with no skipped meals 😀 . I didn’t start with a goal that high, but that reflects where I am now at in my recovery journey.
This helped to eliminate decision making at each meal time. Meal times were often emotionally charged times, filled with intense feelings of anxiety and shame. I have found it better to spend 20 minutes planning several days’ meals than 1 hour speculating over one meal. This also allowed me to decide what I would eat away from the anxiety of meal times and ensured I bought the correct quantity of food in advance – so there’s not too little or too much food in the fridge. Initially, my menu was the same day in and day out, and it took quite some time until I was ready to introduce variety into my week. I now enjoy a variety of foods, but on days where things are a little tougher or a little more emotional, I have my basic meal plan which I can fall back on, to ensure my nutritional needs are met. For a blank menu template, click here or on the image above. For each meal time, there is space to write in what you will have, and then a little column/box next to it to tick off once you have completed that meal. I set goals with my treating team of how many ticks a week I will accomplish and then set rewards for metting these targets. I love playing board games, so my current reward is a new game when I sustain one month with no skipped meals 😀 . I didn’t start with a goal that high, but that reflects where I am now at in my recovery journey.
Developing a healthy relationship with food has been rather challenging. Initially, I had no idea where to start and was not even aware of all my disordered beliefs and behaviours. How did I go about restoring (or perhaps building for the first time) appropriate eating behaviours? There are a few concepts/practices that have really supported me in this regard, so I thought I might share them with you. I have divided them into the following three sections:
- Shane Jeffrey’s R.A.V.E.S principles for nutrition and recovery (Regularity, Adequacy, Variety, Eating Socially, and Spontaneity).
- Top Tips (a list of practical things that have helped me achieve meal completion).
- Meal Support (establishing a network of people who could provide emotional and practical support before, during, and after meals).
 Remember, eating is ESSENTIAL to recovery, and I strongly recommend you find a dietitian who can really support you as you walk your path of recovery. I have had some dietitians that have compounded and fuelled my eating disorder, so if you find that your dietitian does not really understand eating disorders or is unhelpful, don’t lose heart…keep searching – there are some great ones out there! Check out the Directory of Health Professionals for links to some of my favourites.
Remember, eating is ESSENTIAL to recovery, and I strongly recommend you find a dietitian who can really support you as you walk your path of recovery. I have had some dietitians that have compounded and fuelled my eating disorder, so if you find that your dietitian does not really understand eating disorders or is unhelpful, don’t lose heart…keep searching – there are some great ones out there! Check out the Directory of Health Professionals for links to some of my favourites.